 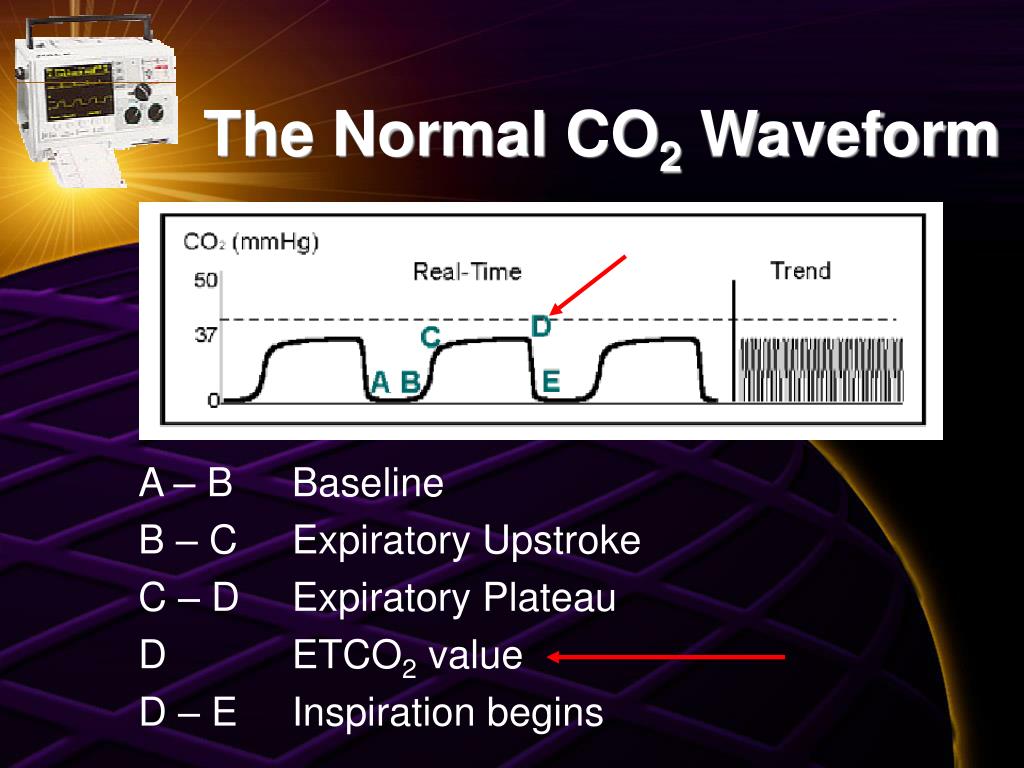 
MAC is a different value for each anesthetic agent. The definition of MAC is the Minimum Alveolar Concentration (%, percent) of the anesthetic that will prevent response to a standard painful stimulus (e.g. Less than MAC will be adequate for maintenance of anesthesia when other agents are administered that provide moderate to severe sedation or good analgesia, for example, premedication with large doses of Domitor or Telazol, or continuous infusions of morphine or fentanyl, or nerve blocks of the surgical site with bupivacaine. Depth of inhalation anesthesia can be regulated by adjusting the vaporizer to maintain patient's end-tidal % at 1.2-1.5 xMAC. End-expiration (end-tidal) concentration approximates alveolar and brain concentrations. Typically the inspired concentration is about 0.2% higher than the expired concentration. The inspired concentration may be the same as the concentration leaving the vaporizer or it may be less, especially in a circle circuit with low oxygen flow and a large dog. 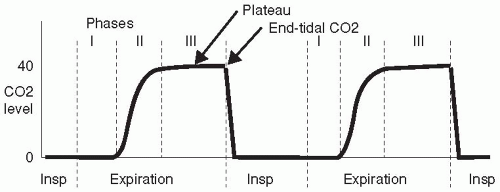
I shall use this information in case discussions to more accurately explain patient assessment and treatment.Īn anesthetic gas analyzer measures inspired and expired anesthetic gas concentrations by aspirating gas from a T-port interposed between the endotracheal tube and the delivery circuit. The monitor is able to fairly accurately determine the concentration of inhalation agent in the patient thus providing information on depth of anesthesia. This monitor is expensive and at present is only available for use in large practices or universities. 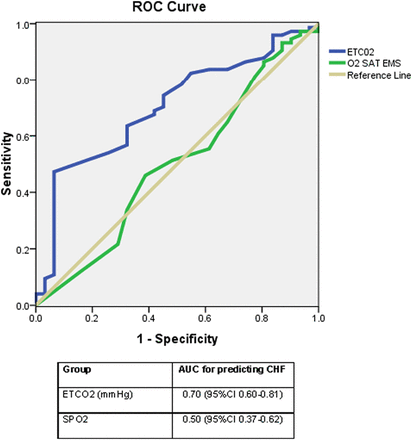
Measurement of alveolar anesthetic gas concentration using an anesthetic gas analyzer. With the addition of Domitor, or as the blood levels of ketamine decrease, the eyeball will rotate. Ketamine maintains muscle tone, thus the eyeball is usually centrally placed in the orbit. If the eyeball is rotated and you can see white of the eye, then severe CNS depression is not present. Most surgical procedures can be performed when the eyeball is rotated in the orbit. In deep anesthesia all the muscles become relaxed and the eyeball returns to the central position. As anesthetic depth increases, the muscles surrounding the eyeball relax at different rates and the eye rotates exposing the sclera or white of the eye. In light anesthesia the eyeball is centrally placed in the orbit. Common recommendations are to monitor several systems and to monitor several parameters of each system and make frequent comparisons of serial recordings.Įyeball movements can be a useful guide to depth of anesthesia with thiopental, propofol, and/or inhalation anesthesia. Monitoring the patient adequately is the basis of safe clinical anesthesia. To emphasis the importance of monitoring from induction to the recovery period.To indicate appropriate treatment for different abnormalities.To discuss examples of anesthetized patients to illustrate evaluation of cardiopulmonary status.To describe the data obtained, normal values, and significance of values outside normal range.To describe the function of commonly available monitors.A decrease in EtCO2 seems to be associated with a higher risk of PEFR ratio less than 50% after treatment. Change in EtCO2 from T60 to T0 was associated with a PEFR ratio less than 50%.Īfter 1 h of treatment, there was no significant change in EtCO2. At T60, 20 (36%) patients had a PEFR ratio less than 50%. There was no significant change in the Q angle and the T time after treatment. There was no significant change in EtCO2 after treatment. The median initial PEFR was 200 the median EtCO2 at T0 and T60 was 35 (IQR: 30-38) and 34 (IQR: 29-37). The mean age was 37 years and 26 (47%) were women. The primary endpoint was the change in EtCO2 the secondary endpoints included changes in the EtCO2 Q angle value, plateau T time, and change in EtCO2 values for the patients with a PEFR ratio less than 50% after treatment.įifty-five patients were included and 36 waveforms were analysed. Data were collected at first medical contact (T0) and after 1 h of treatment (T60). This was a prospective study that included consecutive patients admitted to our emergency department for acute asthma exacerbation. We studied the use of EtCO2 as a monitoring tool in acute asthma. End tidal carbon dioxide (EtCO2) may be considered an accurate surrogate for PaCO2, a severity marker in acute asthma. However, its measurement requires understanding and active participation. The peak expiratory flow rate (PEFR) is the gold standard for monitoring asthmatic patients. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
